A Comprehensive Guide to Contraception Options for Women
SSMTOYS Editorial Team
Release Date: February 28, 2026
Hormonal Contraception Methods: How They Work and Key Options
Combined Hormonal Methods: Pills, Patches, and Rings
Combined hormonal contraceptives contain both estrogen and progestin. They’re often the first choice for many women due to their accessibility and additional health perks.
- Combined Oral Contraceptive Pills (COCs): These are daily pills taken at the same time each day for 21-24 days, followed by a hormone-free week. They come in various formulations, allowing customization for issues like acne or mood swings. Effectiveness with perfect use is over 99%, but typical use drops to about 91-93% due to missed doses. Pros include lighter periods, reduced cramps, and lower risks of ovarian and endometrial cancers over time. For women exploring birth control options for endometriosis symptoms, COCs can provide relief by stabilizing hormone levels. Drawbacks involve potential side effects like nausea, breast tenderness, or a slight increase in blood clot risk, especially for smokers over 35. They’re not ideal for those with a history of migraines with aura, as this could heighten stroke concerns.
- Transdermal Patch: Applied weekly to the skin, the patch releases hormones steadily. It’s a good pick for women who forget pills but want something discreet. Effectiveness mirrors COCs at over 99% with perfect use, though typical rates are around 91%. Advantages include ease of use—no daily routine—and similar menstrual benefits. However, it may cause skin irritation in some, and there’s a minor risk of detachment during activities like swimming. For those researching pros and cons of hormonal patches for busy lifestyles, the patch offers flexibility but requires weekly changes.
- Vaginal Ring: Inserted monthly into the vagina, it releases hormones locally. Perfect use effectiveness exceeds 99%, with typical use at 91%. It’s user-controlled and can be removed briefly for intercourse. Benefits extend to fewer systemic side effects compared to pills, potentially suiting women sensitive to oral medications. Cons include possible vaginal irritation or accidental expulsion. Women considering vaginal ring contraception for minimal daily hassle might appreciate its “set it and forget it” nature for three weeks.
Overall, combined methods shine for regulating cycles but carry a small venous thromboembolism risk, estimated at 7-10 events per 10,000 women-years versus 2-10 without use. They’re reversible, with fertility returning quickly upon discontinuation.
Progestin-Only Hormonal Methods: Pills, Injections, Implants, and IUDs
For women who can’t use estrogen (e.g., due to breastfeeding or hypertension), progestin-only options are safer alternatives.
- Progestin-Only Pills (POPs or Minipills): Taken daily without a break, they thicken mucus and may suppress ovulation. Effectiveness is 99% with perfect timing but 91% typically. Pros: No estrogen-related risks, suitable for postpartum women, and can reduce heavy bleeding. For those looking into minipill birth control for breastfeeding mothers, it’s a top choice as it doesn’t affect milk supply. Drawbacks: Strict timing (within a three-hour window) and irregular spotting.
In clinical settings, we’ve noted that roughly 25-35% of users report breakthrough bleeding in the first few months, but this often diminishes with continued use.
- Injectable Contraceptives (e.g., Depot Medroxyprogesterone Acetate – DMPA): Administered every 12-13 weeks by a provider. Over 99% effective with perfect use, 94% typically. Benefits include privacy and reduced menstrual flow—many experience amenorrhea after a year. It’s practical for women seeking birth control injections for long-term planning without daily reminders. Cons: Potential weight gain (average 2-3 kg), delayed fertility return (up to 10 months), and bone density concerns with prolonged use, though reversible.
- Subdermal Implant: A small rod inserted under the arm’s skin, lasting up to 3-5 years. Effectiveness tops 99%. Advantages: Long-acting, low-maintenance, and highly reliable for forgetful users. For researching contraceptive implants for teens with busy schedules, it’s discreet and effective. Drawbacks: Insertion/removal procedures, irregular bleeding, and rare migration risks.
- Hormonal Intrauterine Device (IUD): A T-shaped device placed in the uterus, releasing progestin for 3-8 years. Over 99% effective. Pros: Minimal user effort, lighter periods (or none), and cramp relief. Ideal for women exploring hormonal IUD options for heavy periods. Cons: Insertion discomfort, possible expulsion, and initial spotting.
To visualize the differences between IUD types, here’s a comparison chart highlighting hormonal and copper options alongside other methods:

Non-Hormonal Contraception Methods: Alternatives Without Hormones
For women preferring to avoid hormones due to side effects or personal reasons, non-hormonal options focus on barriers, spermicides, or natural timing.
Barrier and Chemical Methods
These are used per intercourse, offering on-demand protection.
- Male Condoms: Latex or polyurethane sheaths worn by partners. Typical effectiveness: 82-87%. Pros: STI protection (including HIV), over-the-counter availability, no systemic effects. For couples considering condom use for dual protection against pregnancy and infections, it’s invaluable. Cons: Potential allergies, reduced sensation, and breakage risks.
- Female Condoms: Inserted into the vagina. Effectiveness: 79% typically. Benefits: Woman-controlled, STI prevention. Drawbacks: Noise during use, higher cost.
- Diaphragm or Cervical Cap with Spermicide: Fitted barriers blocking the cervix. Effectiveness: 83-88% with spermicide. Pros: Reusable, non-hormonal. Suitable for women seeking barrier methods for occasional intercourse. Cons: Requires fitting, insertion skill, and UTI risks.
- Spermicides Alone: Chemicals (e.g., nonoxynol-9) in foams/gels. Effectiveness: 72% typically. Advantages: Easy access. Drawbacks: Irritation, no STI protection.
Natural Family Planning and Fertility Awareness Methods (FAMs)
These track cycles to avoid fertile days. Effectiveness: 76-88% typically.
- Withdrawal Method: Partner withdraws before ejaculation. Effectiveness: 78% typically. Benefits: Free, immediate. Drawbacks: Pre-ejaculate risks, reliability issues.
For a clearer understanding of effectiveness across methods, refer to this bar graph illustrating failure rates under typical and perfect use scenarios:
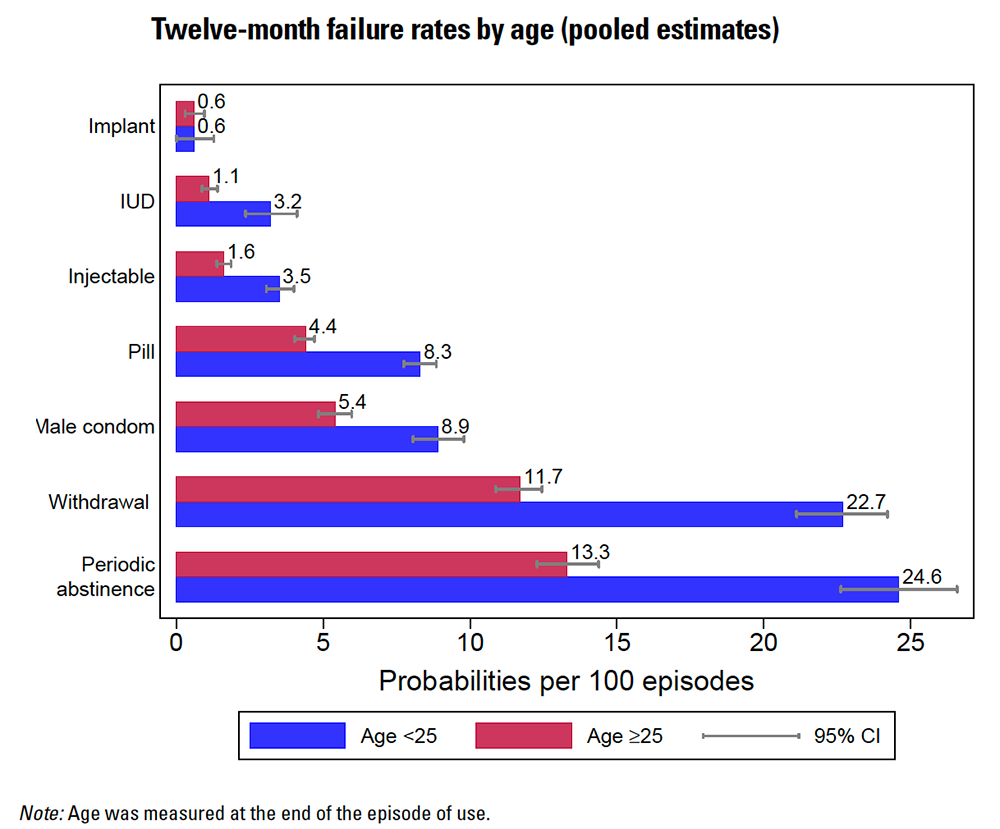
Permanent and Emergency Contraception: Special Considerations
Permanent Methods
- Tubal Ligation: Surgical tying of fallopian tubes. Over 99% effective. Pros: Permanent for completed families. Cons: Invasive, regret risks (especially under 30), no reversal guarantee.
In practice, we counsel that regret rates can reach 20% in younger women, underscoring thorough pre-procedure discussions.
Emergency Contraception
For unprotected sex, options include:
- Levonorgestrel Pills (e.g., Plan B): Over-the-counter, effective within 72 hours (best sooner). 89% reduction in pregnancy risk.
- Ulipristal Acetate (e.g., Ella): Prescription, effective up to 120 hours.
- Copper IUD: Inserted within 5 days, over 99% effective, ongoing protection.
Pros: Backup safety net. Cons: Not for regular use, possible nausea.
Factors to Consider When Choosing a Contraception Method
Potential Health Benefits and Risks Across Methods
Frequently Asked Questions (FAQs)
Here are answers to some common queries based on clinical insights and evidence:
- What contraception is safe during breastfeeding?
Progestin-only methods like minipills, implants, injections, or hormonal IUDs are generally safe and do not impact milk supply. Combined estrogen methods should be avoided until weaning, as they might reduce lactation. Always confirm with your provider. - How soon can I get pregnant after stopping birth control?
For most reversible methods (pills, patches, rings), fertility can return within days to weeks. Implants and IUDs allow quick return upon removal. Injections may delay it by up to 10 months. Track cycles post-discontinuation. - Can contraception help with heavy periods?
Yes, hormonal options like COCs, hormonal IUDs, or injections often lighten flow or lead to amenorrhea. Copper IUDs may increase it, so they’re not ideal for this issue. - What if I have migraines—which methods are safe?
Progestin-only options are preferred, as combined methods with estrogen can increase stroke risk in those with aura. Discuss your history thoroughly. - Are there natural alternatives to hormonal birth control?
Fertility awareness methods or barriers like condoms can work, but they’re less effective (76-88% typically). They require commitment and don’t protect against STIs without additional measures.
